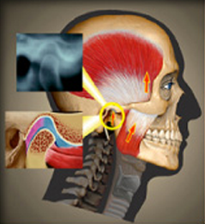
• How would I know if I have a “TMJ” problem?
“TMJ” is not a single disorder but a group of disorders that tend to have a common constellation of symptoms. In other words, these disorders are not all alike. Some are relatively simple; others can be quite complex. Some individuals notice a change in their dental bite associated with the TMJ problem. The symptoms that might accompany a problem of this kind could include one or more of the following:
- • Pain in the face or jaw
- • Pain that seems to be in the ear (may be from the jaw joint)
- • Headaches, particularly when they occur in the temples
- • A feeling of tightness or pain in the jaw upon awakening from sleep
- • Sounds from the jaw joints, such as clicking, popping, grating or grinding
- • Difficulty with opening the jaw (tightness or pain) such as with yawning or at dental visits
- • A sensation of catching or temporary locking of the jaw joint when opening the mouth for talking, yawning, singing or with eating.
An important thing to know is that the symptoms are typically not the actual problem. They are an expression of an underlying condition that is causing the pain. The actual problem usually involves some kind of abnormal function (dysfunction) of the muscles and/or TM joints and other related issues. Treatment that is focused on only relief of symptoms may not adequately address the underlying problem. If “treatment” of this kind should occur, in spite of perhaps achieving short-term relief of symptoms, the actual problem may return, accompanied by the same group of symptoms. Definitive treatment should be focused not only on relieving symptoms but also on addressing the problem that is causing the symptoms. This approach to treatment will be more likely to keep the problem from reoccurring.
• What Causes TMJ?
Temporomandibular Disorders (“TMJ”) represent a broad category of conditions, not a single condition, that tend to have similar symptoms. (Read the previous question and answer) These conditions are frequently a result of more than one factor, which may include hormonal, genetic, dental occlusal, and anatomical factors that may have predisposed the individual to developing a TMD. The actual onset of the symptoms may be insidious (not triggered by any obvious event but developing over time) due to the presence of long-standing predisposing factors.
However, onset can sometimes be precipitated, possibly by trauma, by a bite change, by parafunction (clenching or grinding the teeth), by a whiplash injury, or other factors.
Once the problem has developed, there can also be factors that may prolong or perpetuate the condition, including clenching or grinding of the teeth, bite instability, systemic disease, and age-onset osteoarthritis. A combination of factors, which is often different in each individual, may contribute to the development, and the potential for perpetuation, of these conditions.
To both eliminate the symptoms and to minimize the possibility of the problem returning, it is important that we attempt to identify all of these factors in each patient. Treating not just the symptoms, but also treating the underlying cause of the symptoms, is essential to minimize the possibility of the problem returning in the future.
• My jaw clicks and pops but I don’t have pain. Do I need treatment?
In the general population, a minimum of 30 – 40% of people have clicking or popping sounds in one or both jaw joints. TMJ clicking and popping is common, but it is not normal. When these sounds are present, only one in five people will develop pain or other symptoms, such as catching or locking of the joints. If your jaw clicking/popping has been present for awhile and is not changing over time, you may not need treatment.
But particularly if clicking/popping is becoming louder or more frequent, or if you notice catching in the joint and momentary difficulty opening easily, it is important that you seek knowledgeable help right away. If changes of this kind are developing, be sure to bring this to the attention of your dentist. If you notice that previous joint sounds are no longer occurring, this may indicate that the joint has locked and can be accompanied by pain and limited opening. If the clicking changes to a grinding or grating sound, this may be the start of osteoarthritis of the TMJ. Again, seek knowledgeable dental help, especially if this is accompanied by pain.
• What can I do myself that might relieve my “TMJ” symptoms?
The following are often helpful in temporarily relieving joint and muscle symptoms:
- • Avoid wide or prolonged mouth opening.
- • Eat a soft diet and be careful in other uses of your jaw. Avoid prolonged talking or singing.
- • Take over-the-counter anti-inflammatory medications (maximum dose, if tolerated).
- • Apply moist heat to your face and jaw (hot, moist wash cloths).
Although the symptoms may improve temporarily, using these strategies, the underlying problem that is causing the symptoms is not being addressed by these measures. We strongly recommend that you seek knowledgeable help to diagnose and treat the condition that is causing these symptoms.
• Are my headaches related to my “TMJ” problem?
There are several types of headaches. A few types occur relatively frequently. Others are less common. By far the most common type of headache is referred to as a “tension type” or “muscle contraction” headache. These headaches are characterized by a steady, dull, achy type of pain. They can be episodic or nearly constant. They can also be either relatively mild to very intense. This type of headache can be related to jaw problems or “TMJ” and when they are, they most commonly occur in the temples or behind the eyes. Other “muscle contraction” headaches may occur at other locations and may have other causes. For instance, headaches at the back of the head may be related to tight neck muscles because of poor posture, prior injury, or cervical misalignment. Patients who have “TMJ”-related headaches will very often, but not always, also have headaches at the back of the head.
Another relatively common type of headache is called “migraine” headache and these are typically characterized by a throbbing quality of pain that corresponds to the beating of the heart. For this reason, they are sometimes referred to as “vascular” or “neurovascular” headaches. These can be very severe and debilitating. There are now a number of quite good medications that are effective against true migraine headaches.
Some patients will have a combination of muscle contraction and migraine headache. This is referred to as a “mixed” headache pattern. Each may have its own cause, so a patient with a mixed headache may have a muscle contraction headache that is related to a jaw problem but the migraine portion of the headache pattern may have an entirely different cause. Patients with a mixed headache pattern can often recognize the difference and can tell which one they are having at a given time.
A common misperception is that any headache that is very severe is a “migraine” headache. In spite of a headache being severe, if there is not a throbbing quality to the pain, it may not be a migraine headache. At times, muscle contraction headaches can also be quite severe. The primary distinguishing characteristic of a true migraine headache is the throbbing quality.
Headaches that occur in the temples and that have a steady, aching quality (no throbbing), regardless of the severity, are frequently related to a jaw problem or to problems with your bite. These are problems that can often be managed effectively, once the underlying cause is understood by a knowledgeable dentist.
• I grind my teeth. Can that be treated?
Clenching and grinding of the teeth is known as bruxism and can produce symptoms such as headache, jaw pain, “ear” pain, etc. Because it can also cause damage to the teeth, management of bruxism is often indicated, even if it is not accompanied by pain. There are several possible causes of bruxism, including inadequate restful sleep (see “About Sleep Disorders“) and excessive caffeine or alcohol. Many people who clench and grind their teeth when sleeping also clench or grind when awake. Medications used for improving sleep may reduce bruxism. However, occlusal appliances (“night guards”, “bruxism splints”, etc.) can be useful to prevent tooth damage and have been shown to reduce headaches and facial pain that is caused by the bruxism. Such an appliance will not, however, cause you to quit grinding or clenching. A properly designed occlusal appliance is particularly indicated when there is “ear” pain that may be referred from the temporomandibular joints. When bruxism is accompanied by pain, either muscle pain, pain from the temporomandibular joints, or both, often a “night guard” or “bruxism splint” worn only during sleep will not be sufficient to address the underlying cause of the pain.
Tooth clenching and grinding has previously been attributed to stress. And although stress can certainly be a compounding factor, it is usually not the only factor involved. Patients who carry tension in their jaws often also have neck stiffness and pain. Sometimes problems with the dental occlusion (bad bite) can contribute to the clenching / grinding. Bite problems, as well as stress, may not be the sole cause but a combination of these two can certainly make the clenching and grinding worse.
• Will an over-the-counter (drugstore) device help with my “TMJ” problem?
For uncomplicated jaw problems, some OTC devices may relieve some symptoms on a short-term basis. The style that requires you to bite firmly into a heated material can cause you to hold your jaw in an unnatural, compressed position, which is not helpful. Flexible devices can cause tooth movement. If the device is hard to keep in place at night, this can trigger tooth clenching in your sleep in an attempt to stabilize the device. If you have jaw catching or locking, the problem can be made worse by wearing one of these appliances. For this reason, alone, we recommend that you do not try one of these. It is important to understand that these devices cannot resolve the underlying problem that is causing your symptoms.
• Why do women seek “TMJ” treatment more than men?
Several studies, done in different countries, have clearly shown that women seek treatment for temporomandibular disorders at an average rate of about 7 times greater than men (these studies have varied from 3:1 to 9:1, women to men). However, in studies that have examined general populations groups (not patients), the prevalence of symptoms among women, compared to men, is about 2:1. So it is clear that the conditions that cause TMD symptoms do occur more frequently in women.
Based on age, the occurrence of TMDs in women parallels the child bearing years. This finding strongly suggests that hormonal factors may have a significant influence, perhaps related to an increased extensibility of ligamentous tissues that occur on a monthly basis with menses. Other possible hormonal effects have been proposed, including changes in pain perception related to the menstrual cycle, but at this time there are no firm conclusions that adequately answer this intriguing question.
• What precautions are appropriate during routine dental visits for patients with known “TMJ” problems?
Routine screening of all dental patients has been recommended by the American Dental Association and several other dental organization. This screening can be incorporated into a dental practice fairly easily but few dental offices include this in their routine evaluation of patients. When we lecture to dental groups, we strongly recommend this.
Screening of all patients is the office procedure that allows the clinician to be aware if there is a TMJ problem with each patient and to either treat or refer the “TMJ” patient, hopefully in the early stages of the disorder, before it becomes a more difficult problem. See “Screening for TMDs in Dental Practice“.
With certain temporomandibular disorders, even routine dental care may exacerbate symptoms and/or precipitate progression of an underlying condition. For patients with pain when they open or have a limited range of motion of the jaw, dental procedures of all kinds should be kept to a minimum until the cause has been thoroughly diagnosed and appropriate treatment is undertaken. Elective treatment should be postponed and only critical dental care should take precedence until the TMD concerns have been stabilized. Especially when extractions or other traumatic treatment is necessary, providing support underneath the patient’s jaw during such procedures and keeping the appointments short is recommended. For some patients, placing a small mouth prop that they can close against will reduce muscle fatigue.
• Does insurance cover “TMJ” diagnosis and treatment?
Insurance benefits for temporomandibular disorders varies from no coverage to modest coverage. When benefits are available, they are most likely going to be covered under your medical plan. If you have both medical and dental insurance, in the best of circumstances each may pay a portion of the expense. Because TMD treatment involves joints and muscles primarily, these disorders should be seen as medically comparable to the treatment of other orthopedic joint problems. In that sense, from an insurance perspective, they are typically seen as medical in nature, rather than dental. See “Insurance Benefits for Temporomandibular Disorders (TMDs)”
What kinds of treatment insurance companies cover can also vary greatly. Some will cover diagnostic procedures but nothing else. A few limit coverage to only surgical treatment. Others may cover appliance therapy but not physical therapy or surgical treatment. There does not seem to be any consistent logic behind decisions regarding insurance benefits.
One thing is very clear — decisions by insurance companies regarding benefits are not based on what the individual patient needs. They are primarily based on financial considerations — how large is the premium being paid for the insurance benefits? — larger premium = more benefits. There is additional information regarding insurance benefits elsewhere on this website.