A Discussion for Non-Dental Health Professionals
• How Common Is It? Why Non-Surgical Management?
Health professionals who have not had training in the management of masticatory pain and related symptoms (commonly referred to as “TMJ”) have little reason to appreciate how common these complaints are in the general population. Frequently these disorders are not recognized for what they are. Therefore, appropriate treatment is often delayed. It may not be clear to those outside the dental profession why the comprehensive management of these conditions requires the involvement of a dentist who is thoroughly knowledgable in this unique area of patient care. My purpose here is to briefly explain these disorders.
The preferred term for these conditions is TMDs (plural) – Temporomandibular Disorders. The term refers to a spectrum of conditions involving pain and/or dysfunction of the joints, muscles, and ligaments of the masticatory system. As such, they are similar to other musculoskeletal conditions of the body and in many ways they respond to similar types of treatment. However, unlike other musculoskeletal disorders, the presence of teeth, as a significant influence on the physiologic function of the components of this joint system, both the TM joints and the muscles of mastication, requires an understanding of the unique functional physiology of the jaw system.
• The Sources of Pain in the Jaw System
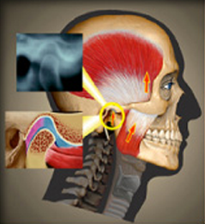
Although the more common term, “TMJ”, derives from “Temporo-Mandibular Joint”, the jaw joints are not the only potential source of pain from the jaw system. In fact, pain arising from the muscles of mastication is more common than pain from the TM joints. This muscular pain may appear as aching in the jaws, and frequently presents as temporalis or frontal headaches. Frequently referred to as “tension” headaches, many of these are associated with problems of the masticatory system.
Onset of a TMD is frequently insidious, although it may be related to a triggering mechanism such as direct trauma to the jaw, or even to injury such as “whiplash”, which produces a rapid and traumatic opening of the jaw, resulting in secondary trauma within the TM joints. TMD should be considered in the differential diagnosis of any persistent pain in the head or facial region. Secondary muscular symptoms in the neck, shoulders, and back are also frequently seen and may be related or may have other causes.
Loss of the normal structural integrity of the TM joints, commonly evidenced by the presence of clicking, popping, or crepitation is present in a minimum of 30-40% of the general population. These joint sounds result when the articular disc, sometimes incorrectly referred to as a meniscus, becomes displaced. Because most in this group appear to live successfully with these sometimes annoying joint sounds, a finding of clicking or popping alone is usually not an indication of a need for treatment. However, in patients who have true joint pain, it is nearly always related to this loss of structural joint integrity. That represents the majority of the patients who come to my office with pain and/or mechanical dysfunction.
It is widely agreed among experts in this field that less than 10% of patients who present with masticatory pain will require surgery of the temporomandibular joints. The remaining 90% or more will respond well to non-invasive therapies when these are effectively executed.
Therefore, in the presence of symptoms of the masticatory system, surgery of the TM joints should be considered only when all reasonable non-invasive therapies have been carefully undertaken and have proven inadequate. Only then, if the pain can be demonstrated to be arising specifically from the temporomandibular joints, should surgery be considered.
• Understanding the Unique Physiology of Masticatory Function
The jaw system, which is the most complex and elegant joint system in the human body, is composed of three major interactive components:
- The temporomandibular joints
- The jaw muscles
- The teeth
In other joint systems of the body, there are only two interactive components; the joint (usually only one), and the muscles that move the joint. There is no other joint system in the body that involves a structure similar to the teeth that can so profoundly affect the function of the joint(s) and muscles of the system.
When anyone with teeth closes their mouth, they will close, with a high degree of precision, to one place — where their teeth fit together best. Because this closure position is so automatic and precise, and because most of us may have lived with it successfully most of our lives, almost everyone will assume that their own bite is “normal” and will usually take for granted that this is the “right” place and manner for the jaw to close.
The ability of the jaw to close in one position with such precision is controlled by a mechanism referred to a neuromuscular engram, which is programmed into the central nervous system by the fit of the teeth. Similar engrams are the basis of learned muscular patterns that we rely on in many other activities requiring muscular coordination, such as riding a bicycle or running up a flight of stairs. Once learned, they become automatic – we don’t have to think about them. If this engram in the jaw system did not exist, we would constantly experience teeth clashing when we talk or chew.
However, this closure position is often a “compensated” position; i.e. a position that avoids destabilizing tooth contacts. As a simple example of compensation: think of walking a mile with a rock in your shoe – the muscular tension that results from repetitively trying to avoid pressure on the rock with each step can lead to pain in the leg and hip. In a similar manner, jaw closure patterns which avoid destabilizing tooth contacts can produce chronic tension in the jaw muscles. This, combined with other factors, can lead to muscular pain. It is often a summation of these various tension-producing discrepancies that eventually leads to muscle pain in the jaws.
Compensation in the jaw system, due to discrepancies of this kind in the dental occlusion, is common. Fortunately, many people seem to adapt to and tolerate these discrepancies in their bite. However, under certain circumstances, chronic compensation combined with the load of functional and parafunctional activities, can lead not only to muscular symptoms but may contribute, in some cases, to structural changes within the TM joints as well, as described earlier.
Although a bite problem may be quite severe, and even in the presence of pain, the patient will seldom recognize that their bite is the source of their problem. Because they have lived with it most of their life, their bite usually feels “normal” to them. Many dentists in this field feel that this compensated jaw closure, which contributes to chronic tension in the jaw muscles, may potentiate patterns of clenching and grinding of the teeth, in yet another way contributing to masticatory muscle pain. In some patients it is evident that bruxism diminishes in response to a more optimum functional environment that can be provided by appropriate treatment.
Although the causation of TMDs has been a subject of debate, the clinical evidence regarding the benefits of dental approaches to treatment can hardly be denied. There is no doubt that a well executed treatment plan, by a knowledgeable dentist, can result in significant relief of muscular and joint symptoms in most patients. But more than that, such a well-executed treatment can establish an environment that will promote a return of functional homeostasis to the dysfunctional masticatory system.
• Dental Oral Appliances
The use of several types of intraoral appliances, when well-designed and used appropriately, have been shown to resolve most muscular complaints. If these appliances are well designed and effectively employed, they can mask the “compensated” detrimental effects of the native bite or “occlusion” and can temporarily produce an optimum occlusal environment, permitting a return of normal physiologic function and contributing to a progressive relaxation of masticatory muscles and a decrease in muscular symptoms. Painful conditions of the temporomandibular joints will also frequently respond to this approach. As the jaw position is allowed to change to one that is more physiologic, inflamed tissues within the TM joints may be unloaded and/or the lateral forces on the joints from bruxism may be reduced. The resulting improved coordination of the muscles can also contribute to improved joint mechanics.
For problems of catching and locking of the TM joints, special appliances that can also provide mechanical control of intracapsular joint mechanics may be employed. Determining the appropriate appliance to be used to accomplish effective management of various masticatory pain problems requires a careful history of the complaint and a comprehensive examination. The effective implementation of any oral appliance relies heavily on the knowledge and experience of the treating dentist for appropriate design, fitting and adjustments.
• Adjunctive Therapy
The management of temporomandibular disorders is certainly not limited to the use of intraoral appliances. The effective implementation and coordination of a variety of adjunctive therapies, chosen to meet the needs of the individual patient, are nearly always essential to expeditiously achieve an optimum result. Perhaps most universally useful is physical therapy by a therapist who is highly knowledgeable and skilled in masticatory management. The level of knowledge and skill that is required is not common. Also useful in certain situations are therapies such as biofeedback, hypnosis, and counseling. Medications to control inflammation and to improve sleep may also be indicated. For more on physical therapy, see “Physical Medicine“.
In cases where surgery may be indicated, effective pre-surgical management, with an oral appliance, together with physical therapy, will usually improve the post-surgical course. And post-surgical rehabilitation should always involve an appropriate appliance and effective physical therapy. It should be evident that the well-coordinated skills of an experienced dentist to quarterback a team of other knowledgeable therapists offers the best opportunity to provide effective treatment for the patient with a difficult temporomandibular disorder.