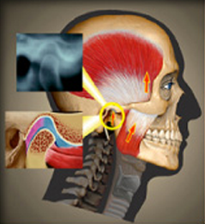
A decades-long discussion (debate) has existed regarding whether occlusal treatment of any kind is necessary or appropriate related to temporomandibular disorders. This debate can be deconstructed into several related questions:
• Is there a relationship between dental occlusion and temporomandibular disorders?
• If such a relationship exists, does dental occlusion play a causative role in TMDs?
• If a causative role has not been clearly established, what is the rationale for doing occlusal treatment?
• If occlusal treatment is indicated, when is it appropriate?
We will address each of these questions individually.
• What is the relationship, if any, between dental occlusion and temporomandibular disorders?
When considering this question, we must be clear that we are defining TMDs not simply as a group of symptoms, but as a loss of normal function (dysfunction) of the masticatory system that may also include pain or other symptoms. The symptoms develop as a result of dysfunction of the components of the masticatory system. Most commonly, these symptoms are expressed in the temporomandibular joints and in the muscles of mastication. It is necessary to understand the mechanisms that would lead to dysfunction of these two key components of a three-component system; TM joints, masticatory muscles, and the role of teeth in the function and loading of the masticatory system.
Unlike any other joint system in the human body, the masticatory system has a third component, the dentition. No other joint system in the human body has a homologue comparable to teeth and the role that the teeth play in the function of the system.
The forces on this load-bearing joint system are generated by the masticatory muscles but are delivered to the system through the teeth. When all the teeth are missing, the load on the system is significantly reduced, even if the patient is wearing full dentures. How the natural dentition contacts, both statically and dynamically, determines how the temporomandibular joints are loaded and also plays a significant role in the amount of force, and the frequency and duration of muscle contraction. For the masticatory system to continue to function in a state of health, with minimal potential for tissue damage, the three components of the system must function in an integrated manner. The role of the teeth in this unique, complex joint system cannot be dismissed as being of little or no significance. When the criteria for appropriate functional loading of the masticatory triad are not met, inappropriate loading can lead to what we refer to as temporomandibular dysfunction.
• What, if any, causative role does dental occlusion play in temporomandibular disorders
There has been a decades-long debate within the dental profession regarding this question. If a causative role of dental occlusion was obvious, research would have, by now, reached some definitive conclusions. In spite of claims by some that the scientific literature does not support a causative role for dental occlusion regarding temporomandibular disorders, a careful reading of the extensive literature tells a different story. First, a very large proportion of that literature is flawed in any of several ways and must be excluded from consideration in addressing the issue of TMD causation. There are only a very small number of studies that meet the exacting standards of science with regard to causation of TMDs. The issues are very complex. The best types of studies are very difficult to do and can be limited by ethical constraints. But the bottom line is that there is currently no strong scientific evidence on either side of the debate regarding the role of dental occlusion as a causative factor in TMDs. A lengthy article by Dr. Higdon explores this complex question in depth. Here is the link to that article.
• If a causative role is not clear in an individual patient, what would be the rationale for doing occlusal treatment?
When an occlusal appliance of an appropriate design is used in the treatment of a temporomandibular disorder, we are primarily altering the occlusal environment so that the masticatory system is being loaded in an optimum manner. In so doing, we are masking the patient’s native dental occlusion, eliminating any adverse loading factors. An occlusal appliance allows us, in most cases, to achieve a stable and pain-free position of the temporomandibular joints within their fossae, thereby achieving an anatomic and functional physiologic relationship between the maxillary and mandibular arches and restoring and stabilizing physiologic function and homeostasis to the system. The consistency with which this outcome is seen makes it difficult to argue that occlusion plays no role in therapy. See “Dental Occlusion and TMDs“.
If the temporomandibular joints, prior to treatment, had not previously been seated in their fossae and/or had been painful to loading or to intrameatal palpation, the use of an occlusal appliance will often result in a favorable change in joint position as the condyles become seated in their fossae. This will be reflected as a change in the dental occlusion. If the therapeutic change in joint position reduces joint pain, this change must be seen as desirable. Integration of the dental occlusion with the joint position means that the occlusal closing position should be consistent with the stable, pain-free seated joint position. The rationale for occlusal treatment, therefore, is to provide this integration in the native occlusion as a means of minimizing the likelihood that the patient will experience a return of the original problem.
• If occlusal treatment is indicated, when is it appropriate? How is this need determined?
Historically, the dental profession used to consider occlusal treatment as the primary treatment for “TMJ.” This may have included equilibration, orthodontics, or restorative dentistry. We now know that occlusal treatment that is undertaken to address the symptoms is getting the cart before the horse. Understandably, this practice gave occlusal treatment a bad reputation with some in the profession. Unfortunately, even now, not everyone is aware that this approach is now considered inappropriate and some continue to attempt to “treat “TMJ”” by initially doing some kind of occlusal treatment.
We now know that occlusal treatment, when it is indicated, should be used only after the symptoms have been largely resolve, and the maxillomandibular relationship (joint position) has been stabilized. This is typically accomplished with the use of an occlusal appliance, supplemented with skillful and effective physical therapy. When these treatment goals have been accomplished and there is evidence of continued stability by means of the occlusal appliance, the occlusal relationships can then be accurately assessed, preferably by means of mounted diagnostic casts. Frequently, due to a seating of the condyles into their fossae, the process of stabilization will often be reflected in a change in the occlusal relationship to some degree. When this is apparent, the goal of occlusal treatment would be to provide a stable, and hopefully functional, jaw relationship that will be consistent with the therapeutically altered jaw (joint) relationship. The rationale for this approach is to eliminate the dental occlusion as a potential perpetuating factor and, thus to minimize the likelihood that an unstable dental occlusion will contribute to a return of the original problem. See “Dental Occlusion and TMDs”